Filariasis, commonly known as elephantiasis, is a debilitating disease caused by parasitic worms. This condition, often acquired in childhood, can lead to severe physical deformities and societal stigma. This blog post delves deep into the symptoms, causes, and management of Filariasis, aiming to provide readers with comprehensive insights into this disease.
Parasitic disease caused by round, coiled, and thread-like worms belonging to the family Filaridea. These parasites penetrate the skin, either on their own or through mosquito bites, eventually reaching the lymphatic system. The disease is primarily caused by the nematode worms, Wuchereria bancrofti or Brugia malayi, and is transmitted by specific mosquito species. This post aims to shed light on the symptoms, causes, and management of this disease.
Symptoms
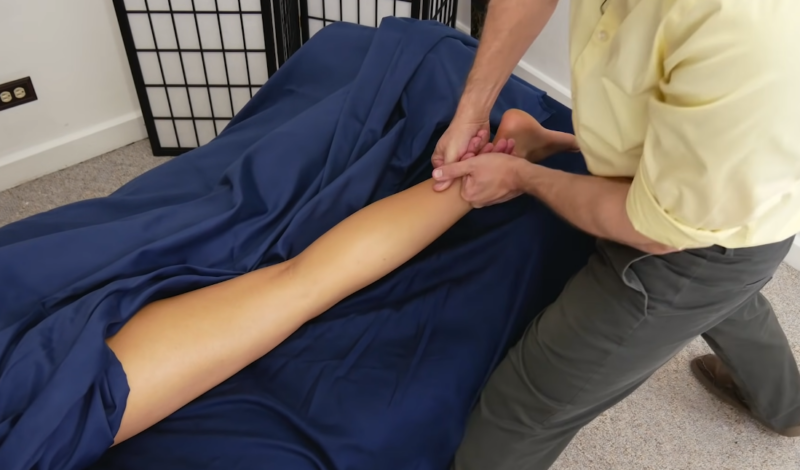
Lymphatic Filariasis (LF) is a condition that can manifest in various ways, ranging from asymptomatic to chronic.
Asymptomatic Stage
The majority of Filariasis infections are asymptomatic, meaning they show no external signs. However, the blood of these individuals tests positive for microfilaria. This silent stage can persist for several months, even though the lymphatic system is already being damaged.
Acute and Chronic Conditions
Acute episodes can involve inflammation of the skin, lymph nodes, and lymphatic vessels. The chronic condition, on the other hand, is characterized by:
- Oedema with thickening of the skin and underlying tissues.
- Swelling, often affecting the lower extremities. However, areas like the arms, vulva, breasts, and scrotum can also be impacted.
- Hydrocele formation in males.
- Enlargement of affected body parts, sometimes several times their normal size, due to blockage in the lymphatic system.
Causes of Filariasis
Understanding the causes of Filariasis is crucial for its prevention and management.
Parasitic Worms
The primary culprits behind most Filariasis cases are the parasites Wuchereria bancrofti and Brugia malayi.
- Wuchereria bancrofti: This parasite is transmitted by mosquito vectors such as Culex, Aedes, and Anopheles.
- Brugia malayi: This parasite is transmitted by Mansonia and Anopheles mosquitoes.
Transmission Cycle
The transmission cycle of Filariasis is intricate:
- An infected mosquito bites a healthy individual, introducing the larvae (microfilariae) into their system.
- These larvae move into the lymphatics and lymph nodes, maturing into adult worms over time.
- Adult worms produce more microfilariae, which circulate in the peripheral blood, especially at night.
- When another mosquito bites the infected individual, it ingests the microfilariae, continuing the cycle.
Diagnosis
Early diagnosis is essential for effective management and treatment of Filariasis.
Blood Sample
Microfilariae, responsible for lymphatic filariasis, circulate in the blood predominantly at night. Therefore, blood collection for diagnosis should be done during nighttime. Samples are then stained and examined under a microscope.
Serological Examination
Serologic techniques offer an alternative to microscopic detection. Patients with active infections typically exhibit elevated levels of antifilarial IgG4 in the blood, which can be detected using specific assays.
Note: Always consult a physician for a comprehensive diagnosis.
Management

Effective management of Filariasis is crucial not only for alleviating the physical symptoms but also for addressing the societal and psychological implications of the disease.
Maintaining Good Hygiene
One of the primary steps in managing Filariasis is ensuring proper hygiene of the affected areas:
- Regularly cleaning and drying the affected parts can prevent secondary bacterial skin infections.
- Elevating the affected limb can help reduce swelling.
- Engaging in regular exercises can promote lymph flow, alleviating some of the symptoms.
Medication and Treatment
Several drugs have shown efficacy in treating Filariasis:
- Mass Drug Administration (MDA): This approach involves administering a single dose of two medicines together. The combination usually includes albendazole (400 mg) with either ivermectin (in areas where onchocerciasis is also prevalent) or diethylcarbamazine citrate (in areas without onchocerciasis). These medicines help clear microfilariae from the bloodstream.
- Alleviating Symptoms: While medicines can treat Filariasis, the persistent enlargement of body parts and associated pain can remain. Physical therapy and surgical interventions might be necessary in some cases.
Psychological and Societal Implications
Filariasis, especially in its advanced stages, can lead to significant societal stigma:
- Affected individuals often face discrimination and isolation due to the visible deformities.
- The psychological toll of the disease can lead to depression, anxiety, and other mental health issues.
- It’s essential for communities to be educated about the disease to reduce stigma and support affected individuals.
Prevention
Prevention is always better than cure, and this holds true for Filariasis:
Mass Drug Administration (MDA)
- Regular MDA campaigns in endemic areas can significantly reduce the disease’s prevalence by interrupting its transmission cycle.
Mosquito Control
- Using insecticide-treated nets and mosquito repellents can prevent mosquito bites, reducing the risk of transmission.
- Environmental management, such as eliminating mosquito breeding sites, can also play a crucial role in controlling the disease’s spread.
Community Awareness
- Educating communities about the causes, symptoms, and prevention of Filariasis can lead to early detection and treatment.
- Awareness campaigns can also help reduce the societal stigma associated with the disease.
FAQ
1. How common is Filariasis worldwide?
Filariasis is more prevalent in tropical and subtropical regions, affecting over 120 million people globally. The World Health Organization (WHO) has identified it as a neglected tropical disease.
2. Can it be fatal?
While Filariasis itself is rarely fatal, complications arising from secondary infections, kidney damage, or severe lymphedema can be life-threatening if not treated promptly.
3. Are there vaccines available?
As of now, there is no vaccine available for Filariasis. Prevention primarily revolves around mosquito control and mass drug administration.
4. Can Filariasis recur after treatment?F
Yes, there’s a possibility of recurrence if an individual is bitten again by an infected mosquito. Regular follow-ups and preventive measures are essential after treatment.
5. How can travelers protect themselves from Filariasis?
Travelers to endemic areas should use mosquito repellents, wear long-sleeved clothing, and sleep under insecticide-treated nets to reduce the risk of mosquito bites.
6. Is it contagious?
No, Filariasis is not contagious and cannot be transmitted from person to person. It spreads only through mosquito bites.
7. Are children more susceptibl?
Children can be more vulnerable due to their underdeveloped immune systems. Moreover, early exposure can lead to more severe complications in adulthood.
Conclusion
Filariasis, while a severe and debilitating disease, can be managed and even eradicated with the right interventions. Through a combination of medical treatments, preventive measures, and community education, we can hope for a world free from the shackles of this disease. Always consult with healthcare professionals for diagnosis and treatment, and remember that early detection is key to effective management.

