Kala-azar, also known as visceral leishmaniasis, is a neglected tropical disease that affects millions of people worldwide, particularly in developing countries. This debilitating disease is caused by protozoan parasites of the genus Leishmania, transmitted to humans through the bite of infected sandflies.
Kala-azar can have severe health consequences if left untreated, making it crucial to understand its symptoms, causes, diagnosis, management, and prevention strategies. In this comprehensive guide, we will delve into the intricate details of Kala-azar, shedding light on its various aspects to empower readers with the knowledge to combat this disease effectively.
Kala-azar, derived from Sanskrit words meaning “black fever,” refers to the darkening of the skin associated with the disease. This name reflects one of the prominent symptoms of Kala-azar, which is an enlargement of the spleen and liver leading to skin darkening.
This parasitic infection is primarily found in East Africa, the Indian subcontinent, and parts of South America, creating a significant health burden in these regions.
Kala-azar is caused by several species of Leishmania parasites, with Leishmania donovani and Leishmania infantum being the primary culprits. These parasites are transmitted to humans through the bite of infected female sandflies, mainly belonging to the Phlebotomus species in the Old World and the Lutzomyia species in the New World.
The Global Impact
Kala-azar is classified as one of the “neglected tropical diseases” by the World Health Organization (WHO). It predominantly affects populations in poverty-stricken areas with limited access to healthcare and proper sanitation.
The disease can have devastating consequences if not addressed promptly, leading to a high mortality rate if left untreated. For more tropical diseases check our article about Amoebiasis.
Recognizing the Symptoms
The onset of Kala-azar is often insidious, with symptoms typically appearing within a few weeks to several months after infection. Early symptoms can be nonspecific and easily mistaken for other illnesses, making diagnosis challenging at this stage. Some common early warning signs include:
- Fever: Recurrent and prolonged fever, often accompanied by chills and sweating, is one of the hallmark symptoms of Kala-azar.
- Fatigue: Profound weakness and fatigue are common and can significantly affect daily life.
- Weight Loss: Unexplained weight loss is a common complaint among Kala-azar patients.
Advanced Symptoms
As the disease progresses, more severe symptoms may manifest, including:
- Enlarged Spleen and Liver: Hepatosplenomegaly, the enlargement of both the spleen and liver, is a characteristic feature of Kala-azar, leading to abdominal discomfort.
- Anemia: Kala-azar can cause severe anemia, leading to pallor and weakness.
- Swollen Lymph Nodes: Lymphadenopathy, or swollen lymph nodes, may occur in some cases.
- Darkening of the Skin: The darkening of the skin, from which the disease gets its name, can become more pronounced.
Causes

The primary causative agents of Kala-azar are protozoan parasites of the Leishmania species. These parasites have a complex life cycle that involves two hosts: the sandfly vector and a mammalian host, usually a human. Here’s a brief overview of how the infection occurs:
- Vector-Borne Transmission: Infected female sandflies, during a blood meal, inject Leishmania parasites into the human host’s bloodstream.
- Migration to Immune Cells: Once inside the body, the parasites are engulfed by immune cells called macrophages.
- Intracellular Survival: Leishmania parasites can evade the immune system by residing within these macrophages.
- Replication and Spread: Within macrophages, the parasites multiply and can spread throughout the body via the bloodstream and lymphatic system.
Factors Influencing Transmission
Several factors contribute to the transmission and prevalence of Kala-azar:
- Environmental Factors: The presence of suitable sandfly habitats, such as stagnant water and organic matter, increases the risk of transmission.
- Human Behavior: Activities that expose individuals to sandfly bites, such as outdoor work and sleeping in open areas, contribute to transmission.
- Malnutrition: Poor nutrition weakens the immune system, making individuals more susceptible to infection.
- Coinfections: Other infections, such as HIV, can increase the severity of Kala-azar.
Diagnosing Kala-azar
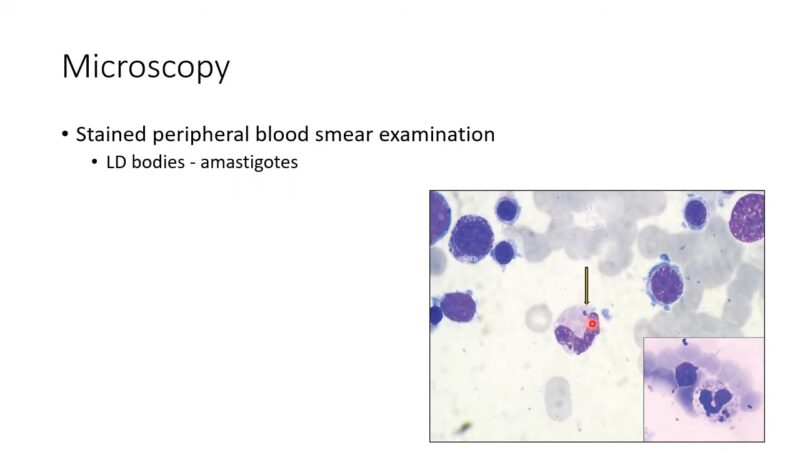
Diagnosing Kala-azar can be challenging due to its nonspecific symptoms in the early stages. However, healthcare professionals use a combination of clinical evaluation and laboratory tests to reach a diagnosis.
The clinical evaluation includes:
- Medical History: Gathering information about the patient’s travel history and exposure to sandfly-prone areas.
- Physical Examination: Checking for enlarged spleen, liver, and other characteristic symptoms.
Laboratory Tests
Laboratory tests are crucial for confirming a Kala-azar diagnosis:
- Blood Tests: These include serological tests like the Direct Agglutination Test (DAT) and the rK39 rapid diagnostic test, which detect antibodies against Leishmania parasites.
- Bone Marrow Aspiration: This invasive procedure involves extracting a sample of bone marrow to detect the presence of parasites.
Managing Kala-azar
Once diagnosed, Kala-azar is treatable, and prompt intervention is essential to prevent complications. Treatment typically involves antiparasitic drugs, such as:
- Sodium Stibogluconate: This medication has been a cornerstone in treating Kala-azar for decades, but its use is declining due to increasing resistance.
- Amphotericin B: This drug, administered intravenously, is highly effective and is often used when other treatments fail.
- Miltefosine: An oral medication that has shown promise in treating Kala-azar.
Monitoring and Supportive Care
Patients undergoing treatment require regular monitoring for side effects and disease progression. Supportive care, including managing anemia and providing nutritional support, is vital for a complete recovery.
Prevention Strategies
Preventing Kala-azar begins with controlling the sandfly vector:
- Insecticide-Treated Bed Nets: Sleeping under bed nets treated with insecticides can reduce the risk of sandfly bites.
- Indoor Residual Spraying: Spraying insecticides inside homes can effectively reduce sandfly populations.
Personal Protection
Individuals living in or traveling to Kala-azar-endemic regions can take steps to protect themselves:
- Wear Protective Clothing: Covering exposed skin, especially during peak sandfly activity hours, can reduce the risk of bites.
- Use Insect Repellent: Applying insect repellent to exposed skin can deter sandflies.
- Stay in Well-Screened Accommodations: Choose accommodations with proper screens on windows and doors.
Disease Surveillance
Active surveillance for Kala-azar cases is essential for early detection and response. Healthcare systems in endemic areas should be vigilant in identifying and treating cases promptly.
Research and Innovation
Efforts to develop a vaccine against Kala-azar are ongoing, with promising candidates in various stages of development. A successful vaccine could be a game-changer in controlling the disease’s spread.
Drug Development
Researchers are also exploring new drug therapies and combination treatments to combat drug resistance and improve treatment outcomes.
FAQ
Is Kala-azar the same as Leishmaniasis?
Kala-azar is a specific form of Leishmaniasis, also known as visceral leishmaniasis. Leishmaniasis is a broader term that encompasses various forms of the disease, with Kala-azar being one of the most severe and potentially life-threatening types.
How are Kala-azar and HIV/AIDS related?
HIV/AIDS weakens the immune system, making individuals more susceptible to infections, including Kala-azar. Co-infection with HIV and Kala-azar can complicate diagnosis and treatment, requiring specialized care.
Can pets transmit Kala-azar to humans?
While pets can become infected with Leishmania parasites, transmission to humans through pets is extremely rare. Sandflies are the primary vectors responsible for transmitting the disease to humans.
Are there long-term effects of Kala-azar even after treatment?
In some cases, individuals may experience post-treatment complications or relapses. Regular follow-up with healthcare providers is essential to monitor and manage any potential long-term effects.
Final Words
Kala-azar is a challenging disease that disproportionately affects vulnerable populations in certain parts of the world. Understanding its symptoms, causes, diagnosis, management, and prevention strategies is crucial for healthcare providers and individuals in endemic areas.
Through continued research, innovation, and global collaboration, there is hope for better control and ultimately the elimination of Kala-azar, reducing its burden on affected communities. In summary, Kala-azar is a complex disease with far-reaching consequences, but with the right knowledge and actions, we can work towards a future where it no longer poses a threat to public health.
By staying informed and supporting efforts to combat Kala-azar, we can make a difference in the lives of those at risk.