Epidemic keratoconjunctivitis (EKC) is a highly contagious viral conjunctivitis that has the potential to spread rapidly and cause significant discomfort. Understanding its causes, symptoms, and management strategies is crucial for both healthcare professionals and the general public.
Epidemic keratoconjunctivitis (EKC) is a viral infection of the eye caused by adenoviruses. It is known for its rapid spread and the significant discomfort it can cause to those affected.
EKC is a form of viral conjunctivitis caused by a group of viruses known as adenoviruses. These viruses are responsible for a range of infections, from those affecting the eyes to those impacting the gastrointestinal tract and respiratory system. EKC is particularly notorious for its ability to cause outbreaks, leading to its name “epidemic” keratoconjunctivitis.
Global Impact
EKC is reported worldwide and is known to occur in epidemics. This means that when an outbreak occurs, it can spread rapidly within communities, schools, or other close-knit groups. Similarly, other infectious conditions, such as the tropical disease Kala-azar, also have significant health implications across various global regions.
Causes
Understanding the causes of EKC is crucial for its prevention and management.
Adenoviruses
EKC is primarily caused by adenoviruses. These are a group of viruses that can cause a range of infections. The serotypes 8, 19, and 37 of adenoviruses are most commonly associated with EKC. However, other serotypes can also lead to the condition.
Transmission
EKC spreads through:
- Direct contact with eye secretions.
- Air droplets.
- Exposure in places like swimming pools.
- Contaminated objects, such as cosmetics or diagnostic instruments in clinics.
Risk Factors
Every individual is susceptible to EKC due to the prevalence of low natural immunity against adenoviruses in the general population. However, adults are more commonly affected. Outbreaks often occur in closed institutions like schools, nursing homes, and hospitals.
Symptoms of EKC
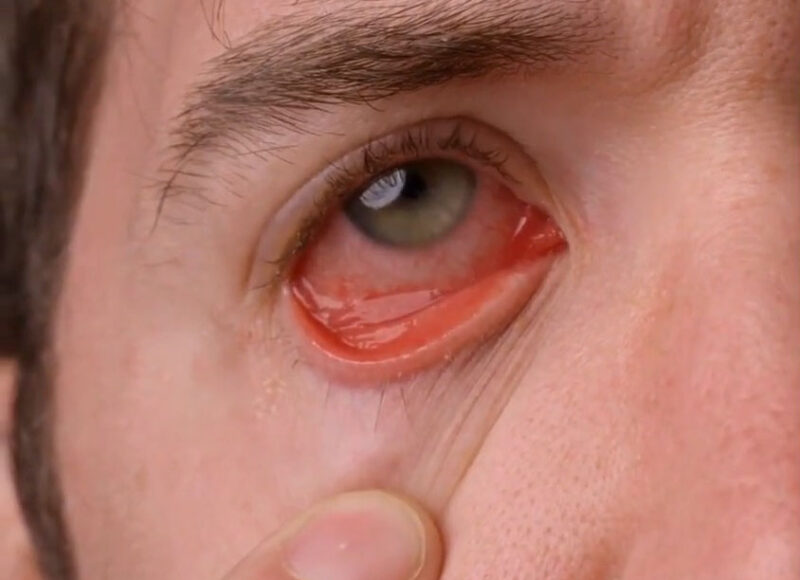
Recognizing the symptoms of EKC is the first step towards its diagnosis and management.
Systemic Symptoms
Before the ocular symptoms appear, individuals may experience:
- Fever
- Headache
- Fatigue
- Swollen lymph nodes, especially in front of the ear
- Respiratory symptoms like coughing or sneezing
- General malaise and body aches
- Digestive symptoms like nausea, vomiting, and diarrhea
Ocular
The eye-related symptoms of EKC can be quite distressing. They include:
- Redness and irritation of the eyes
- Itching and a sensation of having a foreign body in the eye
- Excessive watering of the eyes
- Pain and swelling of the conjunctiva
- Increased sensitivity to light
- Blurred or reduced vision
- Swelling of the eyelids
- Formation of pseudomembranes on the conjunctiva
Diagnosis

Accurate diagnosis of EKC is essential for its effective management.
Clinical
EKC is primarily diagnosed based on its characteristic clinical features. The sudden onset of symptoms, combined with the presence of certain signs like pre-auricular lymphadenopathy (swelling of lymph nodes in front of the ear), can indicate EKC.
Laboratory Tests
Several tests can confirm the diagnosis of EKC:
- Polymerase chain reaction (PCR) assay
- Fluorescent antibody test
- Giemsa cytology, which involves examining stained conjunctival scrapings
- AdenoPlus test, which detects adenoviral particles
Differential Diagnosis
EKC needs to be differentiated from other conditions that can cause similar symptoms. These include trachoma, herpes simplex infection, allergic conjunctivitis, bacterial conjunctivitis, and complications from contact lens use.
Management
While EKC is self-limiting and often resolves on its own, certain management strategies can alleviate symptoms and prevent complications.
Supportive Care
The primary treatment for EKC is supportive care. This includes:
- Cold compresses to reduce swelling and discomfort
- Artificial tears to soothe the eyes
- Topical medications to reduce itching, inflammation, and the risk of bacterial infections
- Cycloplegic agents for severe light sensitivity
Medications
In some cases, medications may be prescribed:
- Mild topical corticosteroids for severe cases
- Topical immune-suppressants, like Tacrolimus, for persistent sub-epithelial infiltrates
- Ophthalmic antiseptics, like Povidone-iodine, to reduce the duration of the disease
Surgical Management
In rare, severe cases, surgical interventions might be necessary. These can include procedures to remove sub-epithelial opacities or address complications like symblepharon.
FAQ
1. Can EKC lead to permanent vision loss?
While it can cause discomfort and temporary vision disturbances, it rarely leads to permanent vision loss. However, if complications arise or if the condition is not managed properly, there could be lasting effects on vision.
2. How can I prevent the spread to my family members?
Avoid sharing personal items like towels, pillows, and cosmetics. Wash your hands frequently, especially after touching your eyes. Stay home when your symptoms are at their peak to prevent spreading the virus.
3. Are there any over-the-counter treatments?
While there are over-the-counter eye drops that can provide relief from symptoms, it’s essential to consult with an eye specialist before using any medication to ensure it’s appropriate for your condition.
4. How long does it take for symptoms to appear after exposure?
The incubation period for EKC is typically between 2-14 days. This means that after exposure to the virus, symptoms can appear within this timeframe.
5. Can I wear contact lenses while I have EKC?
It’s recommended to avoid wearing contact lenses while experiencing symptoms. The lenses can aggravate the condition and increase the risk of complications.
6. Are children more susceptible to IT than adults?
While it can affect individuals of all ages, adults are more commonly affected. However, children can still contract the virus, especially in close-knit settings like schools.
7. Can It recur after recovery?
Yes, it’s possible to get EKC more than once, especially if exposed to the virus again. However, most people develop some immunity after an infection, reducing the chances of recurrence.
Conclusion
Epidemic keratoconjunctivitis is a challenging condition due to its contagious nature and the discomfort it causes. However, with proper understanding, diagnosis, and management, its impact can be minimized. Whether you’re a healthcare professional or someone seeking information, being informed about EKC is the first step towards tackling it effectively.

